Respiratory System
The primary function of the respiratory system is the supply of oxygen to the blood so this in turn delivers oxygen to all parts of the body. The respiratory system does this while breathing is taking place. During the process of breathing we inhale oxygen and exhale carbon dioxide. This exchange of gases takes place at the alveoli. The average adult's lungs contain about 600 million of these spongy, air-filled sacs that are surrounded by capillaries. The inhaled oxygen passes into the alveoli and then diffuses through the capillaries into the arterial blood. Meanwhile, the waste-rich blood from the veins releases its carbon dioxide into the alveoli. The carbon dioxide follows the same path out of the lungs when you exhale.
To put it simply, the principle functions of the respiratory system are:
- Ventilate the lungs
- Extract oxygen from the air and transfer it to the bloodstream
- Excrete carbon dioxide and water vapour
- Maintain the acid base of the blood
Inspired Air
This contains approx:
- 79% nitrogen
- 20% O2
- 0.04% CO2
- Water vapour/Trace Gases
Expired Air
This contains approx:
- 79% nitrogen
- 16% O2
- 4% CO2
- Water vapour/Trace Gases
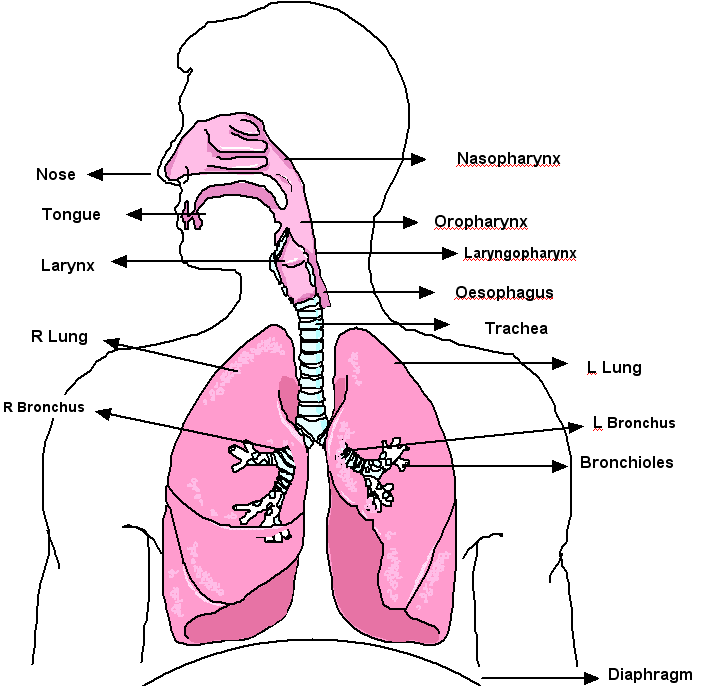
Components of the respiratory System (West, S 2007)
Respiration takes place with the aid of the mouth, nose, trachea, lungs, diaphragm and intercostal muscles . Oxygen enters the respiratory system through the mouth and the nose. The oxygen then passes through the larynx and the trachea. In the chest cavity, the trachea splits into two bronchi. Each bronchus then divides again forming the bronchial tubes. The bronchial tubes lead directly into the lungs where they divide into many smaller tubes which connect to tiny sacs called alveoli.
Nose:
• Olfaction (smelling)
• Assists in producing sound
• Warming and Humidifying. Highly vascularized mucus membrane that warms and humidifies inspired air. Without this function the trachea can become dry.
• Upper one-third of the nasal cavity is lined with olfactory epithelium the lower two-thirds are lined with pseudostratified ciliated columnar epithelium.
• All the way through the respiratory tract there are numerous mucous secreting goblet cells with microvilli on the surface.
• Cilia plays an important role in propelling mucous and trapped particles in to the pharynx where it is swallowed or spat out.
Pharynx:
• Extends from the base of the skull to the inferior border of the cricoid cartilage
• Continuous anteriorly with the trachea and posteriorly with the oesophagus
• Divided into 3 parts; Nasopharynx, Oropharynx, Laryngopharynx.
• Oro and Laryngopharynx are part of the respiratory and alimentary tract and are lined with non-keratinized stratified squamous (NKSS)
Larynx:
• Inferior end continuous with the trachea. Superior end attached to the hyoid bone and lies below the epiglottis
• Protects the trachea from foreign objects and particles.
• Assists in warming and humidifying incoming air
• Made of cartilaginous material
• The larynx is lined with NKSS epithelium as well as pseudostratified ciliated columnar epithelium
• Includes; Epiglottis, Thyroid, Arytenoid and Cricoid cartilages
• Vocal cords are housed in this area. Air rushing past these cords cause them to vibrate thus making sound
Trachea:
• 10cm in length, 2.5cm in diameter and constructed of incomplete C-shaped hyaline cartilage. Rings are completed posteriorly by the trachealis muscle
• Extends from the larynx to the carina; level with 4th and 5th thoracic vertebra
Bronchi:
• Primary bronchi is inferior to the carina; bifurcation of the trachea.
• The bronchi are similar in structure to that of the trachea and are lined with ciliated columnar epithelium. As the tubes become smaller the cartilages become irregular and also become smaller until the tubes get to 1mm, this is when the cartilage disappears. As there is no cartilage the smooth muscle becomes thicker.
Bronchioles:
• No cartilage as the smooth muscle is thicker to help maintain the structure.
• The smooth muscle is responsive to autonomic nerve stimulation
• The internal walls are lined with ciliated columnar mucous membrane but as the walls extend towards the distal bronchiole this membranous layer changes to non-ciliated cuboidal-shaped cells.
Terminal Bronchioles:
• Split into 2 or more respiratory bronchioles
• Thinner walls and are lined with ciliated columnar epithelium.
• Do not contain any goblet cells.
• Increased numbers of clara cells that line the lumen and secrete an agent similar to surfactant
(Waugh & Grant 2004) (GP Notebook 2003) (McGowan, Jefferies, Turley 2004)(West,S 2007)
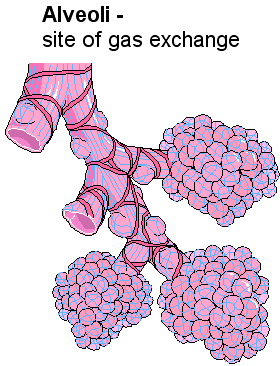
Air from the atmosphere passes through the conducting airway until it reaches the alveoli. The walls of the alveoli are only one cell thick and this is called the respiratory surface, which is about 70 square metres, where the exchange of gases takes place. Around the alveoli are microscopic capillaries that bring carbon dioxide from the heart via pulmonary artery and delivers oxygen back to the heart via the pulmonary vein. Gas exchange happens when there is a difference in partial pressure at the semi-permeable membrane of the alveoli (diffusion). The diffusion occurs when the higher concentration of a gas moves to the lower concentration until equilibrium is achieved (Waugh & Grant 2004).
Gas |
Alveolar |
Deoxygenated Blood |
Oxygenated Blood |
|---|---|---|---|
O2 |
105 mmHg |
40 mmHg |
100 mmHg |
CO2 |
40 mmHg |
44 mmHg |
40 mmHg |
Using the table above, we can see that oxygenated blood from the alveolar will diffuse across the semi-permeable membrane and replace the lower concentration of 02 in the deoxygenated blood. The higher concentration of C02 will diffuse in the same way. This is because Dalton’s law states ‘each gas exerts its own pressure in proportion to it’s concentration in a mixture’. Inhaled 02 has a higher percentage than exhaled 02, its pressure is higher at 100mmHg compared to the 40mmHg of lower percentage from the deoxygenated blood. The reverse of this applies to the C02 because the percentage breathed in is lower than that which is exhaled.(Waugh & Grant 2004) (West,S 2007)
The act of breathing consists of two phases, inspiration and expiration
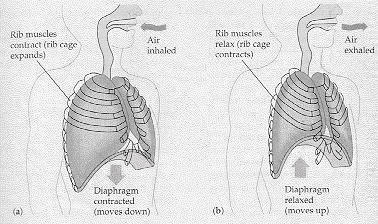
- Inspiration- Diaphragm and intercostal muscles contract. The diaphragm moves downwards. The intercostals muscles make the rib cage move upwards. These two processes increase the volume of the thoracic cavity and also reduces the air pressure to below atmospheric pressure allowing air to rush into the airways then into the alveoli. (Waugh & Grant 2004).
- Expiration is the opposite of inspiration as in the diaphragm and intercostal muscles relax, this allows the diaphragm to move upwards and the intercostal muscles let the rib cage relax to its resting state. The volume within the thoracic cavity now decreases. This decrease in volume now causes an increase in pressure above atmospheric pressure which forces air out up the airway (Waugh & Grant 2004).
Central Control
Breathing is clearly an involuntary process (you don't have to think about it), and like many involuntary processes (such as heart rate) it is controlled by a region of the brain called the medulla. The medulla and its nerves are part of the autonomic nervous system (i.e. involuntary). The region of the medulla that controls breathing is called the respiratory centre. The main centres are the apneustic centre, which enhances inspiration, and the pneumotaxic centre, which terminates inspiration.
The respiratory centre transmits regular nerve impulses to the diaphragm and intercostal muscles to cause inhalation. Stretch receptors in the alveoli and bronchioles detect inhalation and send inhibitory signals to the respiratory centre to cause exhalation. This negative feedback system in continuous and prevents damage to the lungs
Ventilation is also under voluntary control from the cortex, the voluntary part of the brain. This allows you to hold your breath or blow out candles, but it can be overruled by the autonomic system in the event of danger. For example if you hold your breath for a long time, the carbon dioxide concentration in the blood increases so much that the respiratory centre forces you to gasp and take a breath.
Peripheral Chemoreceptors
A chemoreceptor, is a cell or group of cells that transduce a chemical signal into an action potential
Chemoreceptors in the carotid arteries and aorta, detect the levels of carbon dioxide in the blood. To do this, they monitor the concentration of hydrogen ions in the blood, which increases the pH of the
blood, as a direct consequence of the raised carbon dioxide concentration.
The response is that the inspiratory control from the apneustic centre, sends nervous impulses to the external intercostal muscles and
the diaphragm, via the phrenic nerve to increase breathing rate and the volume of the lungs during inhalation.
Respiratory Terminology
- Total lung capacity (TC), about six litres, is all the air the lungs can hold.
- Vital capacity (VC) The maximum volume of air that can be expelled at the normal rate of exhalation after a maximum inspiration
- Tidal volume (TV) is the amount of air breathed in or out during normal respiration. It is normally from 450 to 500 mL.
- Residual volume (RV) is the amount of air left in the lungs after a maximal exhalation. This averages about 1.5 L.
- Expiratory reserve volume (ERV) is the amount of additional air that can be breathed out after normal expiration. This is about 1.5 L.
- Inspiratory reserve volume similarly, is the additional air that can be inhaled after a normal tidal breath in. About 2.5 more litres can be inhaled.
- Functional residual capacity, (ERV + RV), is the amount of air left in the lungs after a tidal breath out.
- Inspiratory capacity (IC) is the volume that can be inhaled after a tidal breath out.
- Anatomical dead space is the volume of the airways.
Further Reading on the Respiratory System
- http://www.leeds.ac.uk/chb/lectures/anatomy7.html
- http://users.rcn.com/jkimball.ma.ultranet/BiologyPages/P/Pulmonary.html
References
GP Notebook, (2003). Terminal Bronchioles. [Online] Available at: http://www.gpnotebook.co.uk/cache/-1543110596.htm (Accessed 6 December 2006)
McGowan P, Jefferies A, Turley A (2004). Crash Course Respiratory System 2nd Edition. London: Mosby
Waugh A, Grant A (2004) Anatomy and Physiology in Health and Illness 9th Edition. London: Churchill Livingstone
West, S refers to myself as this text is from one of my university assignments
Updated April 20th 2009