Abdominal Problems
The abdomen is the body region between the lower ribs and the pelvis that contains many vital organs. Abdominal pain can range from mild to severe, be dull or sharp; acute or chronic. Acute pain is sudden pain. The type of pain, its location, and other symptoms that come with it can help suggest the cause.
Due to the range of possible abdominal emergencies the hospital environment is the best place to be diagnosed as a number of tests may need to be carried out to indentify the cause. The main concern for ambulance personnel is to be able to assess the patient and to see if they are Time Critical and to appropriately manage the emergency until the patient reaches definitive care.
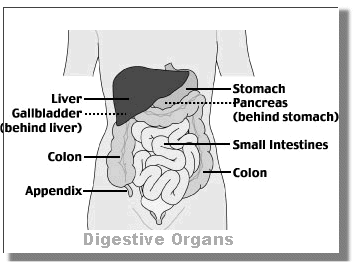
Systems Which Make Up The Abdominal Region
Gastro-intestinal - The gastrointestinal or digestive tract, also referred to as the GI tract or the alimentary canal or the gut, is the system of organs which takes in food, digests it to extract energy and nutrients, and expels the remaining waste
Urinary - The urinary system is a system of organs, tubes, muscles, and nerves that work together to create, store, and carry, urine. The urinary system includes two kidneys, two ureters, the bladder, and the urethra.
Female Reproductive - is any of those parts of the body which are involved in sexual reproduction, namely the vagina, uterus, fallopian tubes and ovaries.
Male Reproductive - is any of those parts of the body which are involved in sexual reproduction, namely the penis, testicles, prostate glands and seminal ducts
Vascular - major blood vessels such as the aorta and inferior vena cava are also considered part of the abdomen, but are located in the part of the abdomen known as the retroperitoneum
Causes of Abdominal Pain
Below are the more serious causes of abdominal pain that you as ambulance personnel may have to deal with:
Abdominal Aortic Aneurysm - Aortic aneurysms commonly occur in the abdominal aorta, as abdominal aortic aneurysms (AAA), where the walls are thinner. These can grow to a large diameter. Some may grow to over 6 inches before rupturing. An abdominal aortic aneurysm can often be palpated by firm pressure above and around the navel as a large, pulsating mass.
Peptic Ulcer - An ulcer of the stomach (called gastric ulcer) or duodenum (called duodenal ulcer). These ulcers can also be caused or worsened by drugs such as Aspirin and other Non-steroidal anti-inflammatory drugs (NSAIDs), also by having periods of an empty stomach. Relief is often sought after intake of food or the use of antacids. Ulcers are a common cause of internal bleeding.
Kidney Stone - are solid crystals of dissolved minerals in urine found inside the kidneys or ureters, they typically leave the body in the urine stream. As long as they stay within the kidney problems are relatively rare it is when they leave the kidney and start to move down the ureter stretching their wall. This pain will often be collicky in nature and associated with haematuria, nausea and vomiting. Pain is said to be very severe and paramedic assistance may be required to administer strong opiate pain relief.
Diverticulitis - Small pouches in the colon that bulge outwards through weak spots. Each pouch is called a diverticulum. Faecal matter leaks through the thin walls and causes inflammation, on a few occasions this can causes abcesses to develop in the colonic structure. It is when these pouches become infected or inflamed, the condition is called diverticulitis.
Internal Bleeding - Signs and symptoms will include, haematemesis, rectal bleeding, unexpected vaginal bleeding. The fresher the blood the brighter red it will look. e.g. an upper oesophageal bleed will be bright red where old blood will show as coffee grounds.
Abdominal Assessment
Firstly just look at the abdomen and note anything unusual. Mentally note how the abdomen looks is it, concave, flat, rounded, or obese in size. Are there any noticeable scars or new wounds present, which may indicate past, or recent surgery or trauma. Abnormal observations of the exposed abdomen would include an asymmetric contour, prominent veins or pulsation, oedema, rashes, or a steadily increasing size of girth.
Palpate the abdomen with the pads of your fingers, not your finger tips as this can cause pain to the patient. Don't palpate the painful area straight away, palpate other areas of the abdomen first to assess the full extent of the pain.
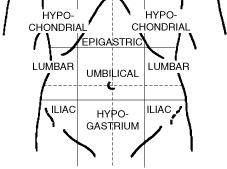
The diagram above shows the different regions of the abdomen so when you handover to hospital staff you'll be able to pinpoint the pain to a certain area.
Some Signs and Symptoms of Abdominal Problems
- Pain
- Nature of Pain - Pain can be constant or colicky. Constant pain usually originates from a solid organ such as the pancreas. Whereas colicky pain lasts for a short period (seconds or minutes), then eases off before returning.
- Fever
- Haematemesis
- Vomiting blood. The blood can be fresh and red (usually bleeding above the gastro-oesophageal sphincter) or when it has been degraded by gastric juices can resemble 'coffee grounds'.
- Melaena
- Vomiting
- Back and Side pain
- Frequent and/or painful Urination
- Signs of Pregnancy
- Haematuria
- Nausea
- Diarrhoea
- Pulsating Abdominal Mass
- Vaginal Bleeding/Discharge (Gain a menstrual history)
- Painful Intercourse
- Rebound tenderness (Not thought to be a reliable indicator of peritoneal irritation)
- Bowel Habits
- Abdominal Distension
- Abdominal Distension is principally caused by the 5 F's: Fat, Flatus, Faeces, Fluid, Fetus.
- Swelling
Named Clinical Signs
- Murphy's Sign - A sign of acute cholecyctitis as you gently palpate the right upper quadrant (RUQ) of the abdomen, while asking the patient to take a deep breath, will illicit a sudden inspiratory 'catch' as the gall bladder descends down and contacts with your fingers due to the diaphragm lowering and pushing gallbladder downwards.
- Iliopsoas Sign - The patient is asked to flex their right thigh against the resistance of your hand. If this causes a painful response in the abdomen then this indicates an inflammatory process has affected the psoas muscle in e.g appendicitis or a perinephric abcess.
- Rovsings Sign - While palpating the left iliac fossa (LIF) may produce pain in the right iliac fossa (RIF) if a patient has acute appendicitis
- McBurney's sign - Deep tenderness at McBurney's point is a sign of acute appendicitis. Specific localisation of tenderness to McBurney's point indicates that inflammation is no longer limited to the lumen of the bowel (which localizes pain poorly), and is irritating the lining of the
peritoneum at the place where the peritoneum comes into contact with the appendix.
- McBurney's point is the name given to the point over the right side of the abdomen that is one-third of the distance from the anterior superior iliac spine to the umbilicus (navel). This point roughly corresponds to the most common location of the base of the appendix where it is attached to the cecum.
- Aaron's Sign - is a referred pain felt in the epigastrium upon continuous firm pressure over McBurney's point. It is indicative of appendicitis.
Management
If any time critical features such as; suspected ruptured or leaking aortic aneurysm, traumatic injury causing disruption to the liver and spleen, ectopic pregnancy or sepsis secondary to perforation are present then correct any A and B problems and transfer to appropriate hospital.
Pain often accompanies abdominal emergencies. To help indentify what may be going on it is important to ask the following questions:
- P - Provocation (What were you doing at time of pain. What makes it worse/better)
- Q - Quality (What the pain feels like? Dull, Sharp)
- R - Radiation (Is the pain felt anywhere else e.g. does it radiate into back, groin)
- S - Severity (Score pain from 0 to 10)
- T - Time (How long has pain been present and how quickly was onset?)
- A - Associated signs and symptoms (Pyrexia, Nausea, Diarrhoea, Constipation, Acid indigestion)
- S - sight of pain and whether it radiates
- O - Onset of pain and whether it's new pain
- C - Characteristics of pain e.g. Constant, intermittent. Has it got worse or better?
- R - Radiates, does pain radiate elsewhere
- A - Associated symptoms such as dizziness, nausea or vomiting
- T - Time the pain started
- E - Exacerbation or relieving factors
- S - Severity. Gain a pain score out of 10
Always consider the administration of Entonox for adequate pain relief pending examination (ascertain what pain relief has been taken by patient), 12 lead ECG monitoring in the elderly or those with cardiac risk factors if presenting with upper abdominal pain, treat for shock if large quantities of blood are believed to have been lost, call for paramedic backup if required.
NOTE: The new JRCALC 2013 No Longer makes reference to Entonox being a caution in the use of abdominal pain where a patient may have abdominal distension/obstruction. Please bear this in mind whenever Entonox is given to you patient as there could be a potential increase of a gas pocket caused by the nitrous oxide.
ASHICE (consider)
Transport to hospital
Professional handover
Updated March 2014